Joint Pain in Women What It Could Mean in Your 40s and 50s

Woman Experiencing Hand Joint Pain
Joint pain often appears in women during their 40s and 50s. It may start as stiffness in the fingers in the morning, aching knees after climbing stairs, or shoulder discomfort that does not ease with rest.
Many people dismiss these symptoms as part of ageing because they develop slowly. However, joint pain is not always due to wear and tear. In some cases, it may signal autoimmune or inflammatory conditions that need specialist care.
Understanding the difference matters.
Mechanical Versus Inflammatory Joint Pain
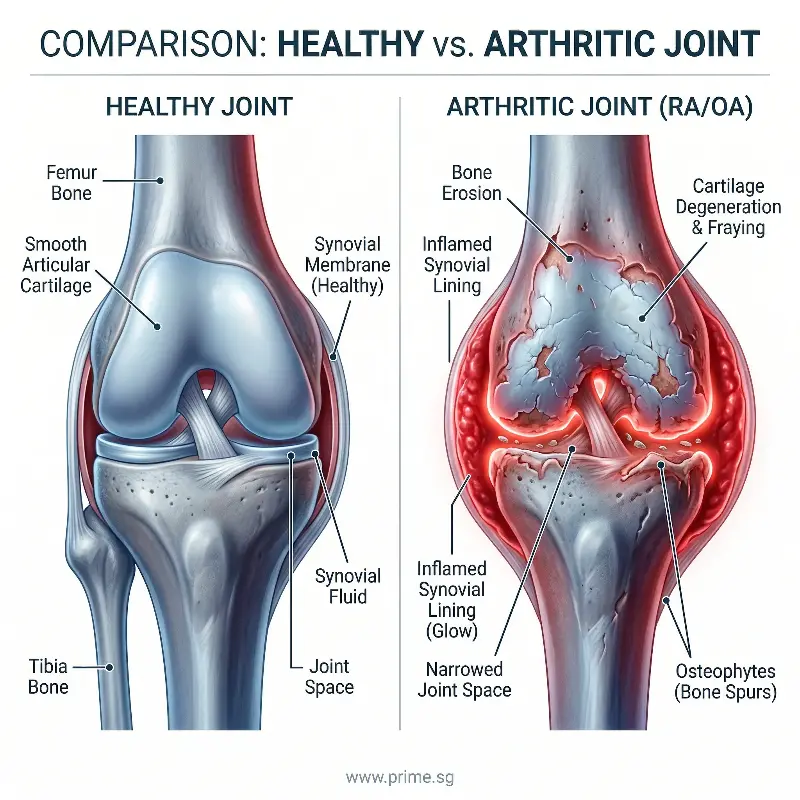
Doctors generally classify joint pain into two main types: mechanical and inflammatory.
Mechanical pain, such as osteoarthritis, develops when cartilage wears down over time. This type of pain usually worsens with movement and improves with rest.
In contrast, inflammatory joint pain occurs when the immune system attacks the joint lining. This leads to swelling, stiffness, and discomfort that follow a different pattern.
Recognising these patterns helps guide the right treatment.
Osteoarthritis The Common Mechanical Cause
Osteoarthritis is the leading cause of joint pain in midlife. It develops gradually as cartilage becomes thinner.
Common symptoms include:
- Pain during movement
- Stiffness after sitting for long periods
- Reduced range of motion
- Mild swelling
Morning stiffness tends to be brief and improves once you start moving.
Although osteoarthritis can cause discomfort, it is not an autoimmune condition. Treatment focuses on exercise, muscle strengthening, and maintaining a healthy weight.
Rheumatoid Arthritis An Autoimmune Disease
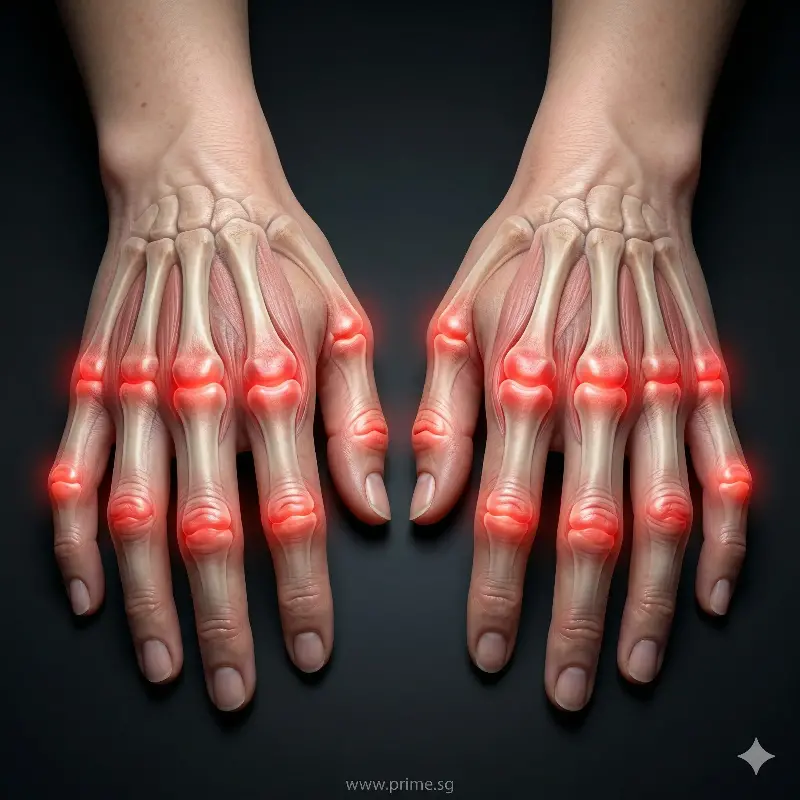
Rheumatoid Arthritis Symmetrical Hand Inflammation
Rheumatoid arthritis is a systemic autoimmune disease. Instead of protecting the body, the immune system attacks the joints, causing inflammation.
This condition affects women more often than men and typically begins between ages 30 and 60.
Key warning signs include:
- Morning stiffness lasting more than 30 minutes
- Swelling in multiple joints
- Symmetrical involvement (both hands or both wrists)
- Warm, tender joints
- Ongoing fatigue
Unlike osteoarthritis, this condition often affects several joints at once and may come with general symptoms like tiredness.
Without treatment, inflammation can damage cartilage and bone. Early diagnosis allows doctors to control inflammation and prevent long-term damage.
Other Autoimmune Conditions That Affect Joints
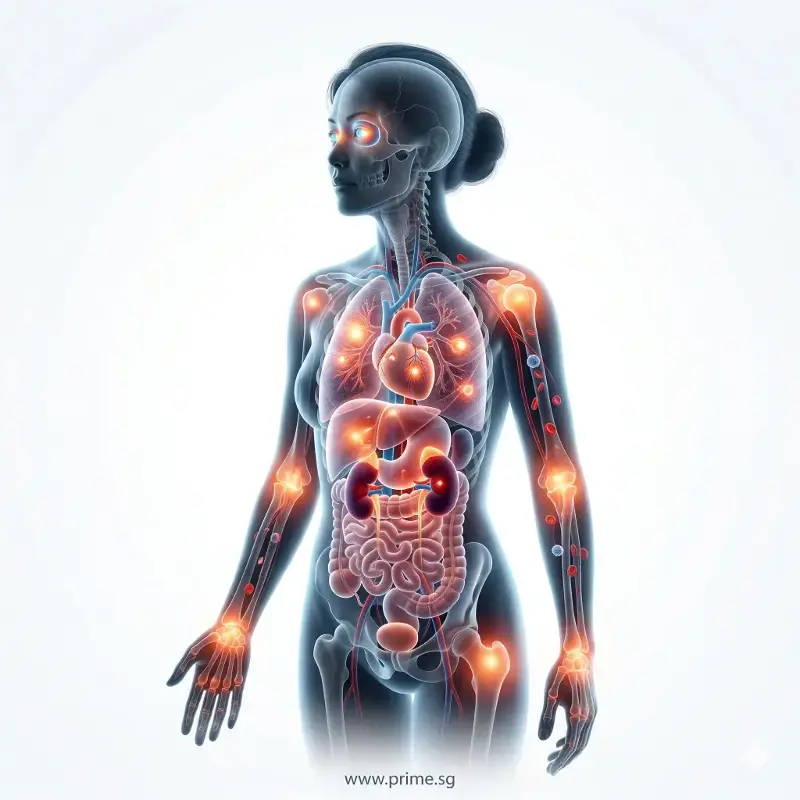
Autoimmune Diseases That Cause Joint Pain in Women – Lupus, Psoriatic Arthritis and More
Joint pain in women may also be linked to other autoimmune diseases such as:
- Systemic lupus erythematosus
- Psoriatic arthritis
- Ankylosing spondylitis which is also more common in men
- Sjogren Syndrome
- Systemic sclerosis
- Myositis
These conditions may involve not only joints but also skin, eyes or internal organs. Joint symptoms may be one of the earliest signs.
Because autoimmune diseases can overlap and present subtly, specialist assessment is often required for accurate diagnosis.
Gout A Metabolic Inflammatory Condition
Gout is not autoimmune, but it is inflammatory. It occurs when uric acid levels rise and crystals deposit in joints, triggering intense inflammation.
Although more common in men, gout can affect women, particularly after menopause.
Features include:
- Sudden severe joint pain
- Redness and swelling
- Recurrent flare ups
Gout attacks may mimic other inflammatory arthritis conditions, making proper evaluation important.
When To See A Rheumatologist
A rheumatologist specialises in diagnosing and managing autoimmune and inflammatory joint diseases.
Medical review should be considered if:
- Morning stiffness lasts longer than thirty minutes
- Swollen and painful joints
- Joint pain is accompanied by fatigue
- Pain persists for several weeks without improvement
While general practitioners can initiate assessment, rheumatologists are trained to differentiate between mechanical joint problems and immune mediated disease.
Early referral matters because autoimmune arthritis responds best when treated promptly. Delayed treatment may allow irreversible joint damage.
Why Early Evaluation Makes A Difference
Consultation with Rheumatologist
Autoimmune joint diseases are driven by inflammation that may not always be visible externally. Blood tests, imaging and clinical assessment help clarify the diagnosis.
Modern therapies can significantly reduce inflammation and prevent long term complications. The goal is not only pain relief but preservation of joint structure and overall function.
For women in midlife, early recognition protects mobility and independence in later years.
Joint Pain Is Not Always Just Ageing
While hormonal changes and mechanical strain contribute to joint discomfort in the 40s and 50s, persistent or inflammatory symptoms should not be ignored.
Understanding whether joint pain is mechanical, metabolic or autoimmune allows targeted treatment.
Seeking specialist advice when warning signs are present can prevent long term damage and support continued quality of life. PRIME
Medical Disclaimer
This article is intended for general educational purposes only and does not constitute medical advice. Consultation with a licensed medical practitioner is recommended for personalised assessment and treatment.
